Lower Back Pain Support in Mentone
Lower Back Pain
Lower back pain changes how you move, work, sleep, and get through your day. It is one of the most common reasons people visit a physiotherapist, and most of the time, the outlook is far better than you might expect.
At mhealth in Mentone, we take the time to understand what’s driving your symptoms and build a management plan that actually fits your life. Not a generic set of exercises printed from a template. A plan that considers your goals, your body, and where you want to get back to.
Whether this started last week or keeps coming back every few months, our team can help you make sense of what’s going on and move forward with confidence.
What Is Lower Back Pain?
Lower back pain refers to discomfort, stiffness, or pain felt anywhere between the bottom of your ribs and the top of your legs. It affects roughly 1 in 6 Australians at any given time, and about 80% of people will experience it at some point in their lives.
Here’s what most people don’t hear often enough: the vast majority of lower back pain is not caused by serious damage. Muscles get irritated. Joints get stiff. Nerves can become sensitive. These things respond well to the right management, and getting started early tends to make a real difference.
Common Symptoms of Lower Back Pain
People describe their lower back pain in all sorts of ways. Some of the most common presentations we see at mhealth include:
- A dull ache or stiffness across the lower back, especially first thing in the morning
- Pain that gets worse with bending, lifting, sitting for long stretches, or standing in one spot
- Sharp or catching pain during sport or physical activity
- Stiffness that eases once you start moving but returns after rest
- Pain that disrupts sleep or wakes you during the night
When the Pain Spreads: Sciatica and Nerve-Related Symptoms
Sometimes lower back pain doesn’t stay in the back. If a nerve becomes irritated, you might notice:
- Pain that travels into the buttock, down the thigh, or below the knee (often called sciatica)
- Pins and needles, tingling, or numbness in the leg or foot
- A feeling of weakness, such as difficulty lifting your foot when walking
If you’re experiencing leg weakness, changes to bladder or bowel function, or numbness in the saddle area, this warrants urgent medical review. These symptoms are rare, but they need same-day attention.
Common Causes of Lower Back Pain
There’s rarely one single cause. Lower back pain is usually the result of several factors working together, and understanding those factors is what helps us build a treatment plan that works.

Muscle and joint irritation is probably the most common driver. The joints and muscles of the lower back can become irritated from overload, poor movement patterns, or simply doing too much too soon. This is especially common after a sudden increase in gym work, sport, or physical activity you're not used to.

Disc-related pain is another frequent contributor. Discs sit between the vertebrae and act as shock absorbers. They can bulge or become irritated, sometimes pressing on nearby nerves. But here's the part that surprises people: disc bulges show up on MRI scans in a large percentage of people who have zero pain. A systematic review found disc bulges present in 30% of 20-year-olds and up to 84% of 80-year-olds with no symptoms at all. Your physiotherapist can help determine whether imaging findings are relevant to your symptoms, or just normal changes that happen with age.

Nerve irritation (sciatica) happens when a nerve root in the lower back becomes compressed or sensitised. It often produces pain, pins and needles, or numbness that travels down the leg. Sciatica treatment typically involves a combination of hands-on therapy, specific exercises, and load management.
Prolonged sitting and postural stress play a role for many people, particularly those working desk jobs. The back isn't designed to be still for 8 hours a day. Prolonged positions create sustained load on certain structures, and over time, that adds up.

Deconditioning matters more than most people realise. After a period of inactivity, illness, or simply not exercising, the muscles that support your spine lose strength and endurance. This makes the back more vulnerable to flare-ups when you return to normal activity.
Lower back pain is more common in desk workers, parents lifting young children, active adults returning to sport, and older adults wanting to stay active. It is also one of the leading causes of early retirement in Australia, with chronic back pain accounting for a significant share of disability and workforce dropout. Load, stress, sleep quality, and general activity levels all influence how your back feels on any given day.
Types of Lower Back Pain
Not all back pain behaves the same way, and recognising the pattern can help guide the right approach.

Acute lower back pain comes on suddenly and usually settles within a few weeks with appropriate management. It often follows a specific event, like lifting something heavy, an awkward movement, or a spike in training load.

Chronic lower back pain is pain that persists beyond 12 weeks. This doesn't mean the back is damaged. Chronic pain is often driven by a combination of physical, lifestyle, and nervous system factors. It responds well to structured rehabilitation that addresses all of these elements.

Recurrent lower back pain is a pattern where pain comes and goes. You might feel fine for weeks or months, then a flare-up hits. This pattern usually indicates underlying factors like strength deficits, mobility limitations, or load management issues that haven't been addressed.

Referred pain and radiculopathy occur when structures in the lower back refer pain elsewhere, often into the buttock, hip, or leg. Radiculopathy specifically involves a nerve root and may produce pins and needles, numbness, or weakness. The treatment approach differs depending on whether symptoms are purely referred or involve nerve compression.
Frequently Asked Questions About Lower Back Pain
Do I need a scan before starting treatment?
Most lower back pain does not require imaging to begin treatment. Choosing Wisely Australia and the Royal Australian and New Zealand College of Radiologists both advise against routine imaging for non-specific low back pain, as trials have found no advantage and some potential harms. Your physiotherapist will assess your movement, strength, and symptoms to determine the most likely cause. Scans are recommended when specific red flags are present or when progress stalls despite appropriate treatment.
Is rest the best thing for my back?
No. Prolonged rest can actually slow your recovery. The Australian Physiotherapy Association recommends staying active and returning to usual activity as soon as possible. Your physiotherapist will guide you on what movements are safe and how to gradually increase your activity levels without aggravating your symptoms.
Can a disc "slip" out of place?
Discs don’t slip. They’re firmly held in place by ligaments, muscles, and the vertebrae themselves. The term “slipped disc” is misleading. Discs can bulge or become irritated, but most disc-related issues improve with the right rehabilitation and don’t require surgery.
Will my back pain come back?
With the right management, most people return to full function. Building long-term strength and resilience through progressive exercise is the best protection against recurrence. Our goal at mhealth is not just to get you out of pain, but to reduce the chance of it returning.
Does lower back pain mean my spine is weak or damaged?
The spine is a strong, adaptable structure. It’s designed to bend, lift, twist, and carry load. Pain doesn’t necessarily mean damage. It often means something has become irritated or overloaded, and with progressive strengthening, the back adapts and becomes more resilient.
When should I see a physio for lower back pain?
If your pain has lasted more than one to two weeks, keeps coming back, limits your ability to work, sleep, or exercise, or involves pain, numbness or weakness into the leg, it’s worth getting an assessment. You don’t need a referral to book with a physiotherapist.
References
- Australian Institute of Health and Welfare (2024). Back problems. Chronic musculoskeletal conditions report.
- Brinjikji, W. et al. (2015). Systematic Literature Review of Imaging Features of Spinal Degeneration in Asymptomatic Populations. American Journal of Neuroradiology, 36(4), 811-816.
- Choosing Wisely Australia. Low Back Pain Hub. Recommendations from RANZCR, APA, and Faculty of Pain Medicine.
- NSW Agency for Clinical Innovation. Low Back Pain Resources. Management of people with acute low back pain.
- Australian Physiotherapy Association (2022). Clinical Care Standard for Low Back Pain. Endorsed by 19 professional associations.
- Australian Physiotherapy Association. Low back pain: what works and what doesn’t.
Painaustralia. Back Pain. Forms of Pain resource.
Lower Back Pain Articles
Not all back pain behaves the same way, and recognising the pattern can help guide the right approach.

Low-Impact Exercises for Back Pain: 9 Pain-Free Ways to Stay Active
If a hard workout leaves you sore for days, the fix usually isn’t to stop moving. It’s to move differently. This guide runs through nine low-impact exercises for back pain and sore joints, from walking and swimming to clinical Pilates, plus how to tell when it’s worth checking in with a physio first.
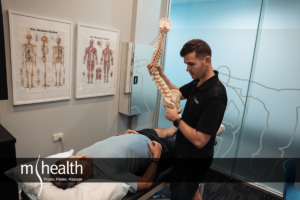
Lower Back Pain MRI: When Scans Help, and When They Don’t
Most people with lower back pain don’t need a scan before starting treatment. Find out when a lower back pain MRI is genuinely useful, what research shows about disc bulge findings in pain-free people, and what to do instead.

Lower Back Pain Causes: A Practical Guide to Working Out What’s Going On
Lower back pain shows up in dozens of ways, and the cause isn’t always obvious. This guide walks through the six most common reasons your lower back might be hurting, from muscle strain and disc irritation to posture pain and training-related injuries, plus the warning signs that mean it’s worth booking an assessment rather than waiting it out.
How mhealth Treats Lower Back Pain
The most effective approach to lower back pain treatment is active, individualised management. The NSW Agency for Clinical Innovation recommends early physiotherapy referral, patient education, and encouraging movement over rest. Passive treatment alone, or a one-size-fits-all approach, rarely produces lasting results. That’s something our team feels strongly about.
Assessment: Understanding Your Back
Your care at mhealth begins with a thorough assessment. We look at how you move, test your strength and mobility, assess your posture, and identify contributing factors like training load, work demands, stress, and sleep.
For the lower back specifically, we’ll often assess your thoracic spine and hips as well. Stiffness or weakness in these areas commonly contributes to lower back symptoms. We may use functional movement tests, such as squats or lifting patterns, to see how your body manages real-world demands.
Where relevant, we use technology like our AXIT strength assessment system and Med-X machine to gather objective strength data. This helps us set meaningful benchmarks and compare your results to normative data for people of a similar age and activity level.
Hands-On Treatment
Manual therapy is a useful part of the physiotherapy toolkit for lower back pain relief. Techniques like joint mobilisation and soft tissue work can help reduce pain and stiffness in the short term, allowing you to move more freely and progress into exercise sooner.
That said, hands-on treatment is rarely recommended in isolation. The evidence is clear: combining manual therapy with active rehabilitation produces better long-term outcomes than either approach alone.
Individualised Exercise Therapy
This is the backbone of what we do. Every exercise plan at mhealth is built around your specific assessment findings and your goals.
Common areas of focus include strengthening the glutes, trunk, and posterior chain, though what gets prioritised depends entirely on your presentation. We also address hip and thoracic mobility where needed, and use gradual load progression to build your body’s capacity over time.
Functional movement retraining is part of this process. The aim is to get you back to doing the things that matter to you, whether that’s picking up your kids, getting back to the gym, or returning to competitive sport.
Clinical Pilates for Lower Back Pain
All clinical Pilates at mhealth is individualised. After a few one-on-one sessions to teach you the exercises and ensure correct form, you’ll transition into a class setting where the exercises are still specific to your goals and presentation.
Pilates for lower back pain can help with motor control retraining (re-teaching your body to activate the right muscles), building core endurance, improving mobility, and progressive resistance work to develop lasting strength.
Education and Load Management
Understanding your condition is part of getting better. We spend time explaining what’s happening, why, and what you can expect during recovery.
Practical education includes safe bending and lifting strategies, graded exposure to movements that might feel uncomfortable, flare-up management plans for those difficult days, and clear guidance around returning to work or sport.
If onward referral to another medical specialist is appropriate, we’ll facilitate that too.
Return to Activity Programs
Getting out of pain is only half the job. We develop structured return-to-activity programs based on what you want to get back to:
- Gym return programs with progressive loading
- Running progression plans
- Strength training integration
- Cycling or sport-specific rehabilitation
Who Is Most at Risk of Lower Back Pain?
Certain factors increase the likelihood of developing lower back pain. Some you can change, others you simply manage around.
Modifiable risk factors:
- Prolonged sitting or sedentary work habits
- Sudden increases in lifting, gym work, or sport
- Poor sleep quality
- High stress levels
- Low overall physical activity
- Reduced hip or thoracic mobility
- Weakness in the core, hips, and legs
Non-modifiable risk factors:
- Previous history of back pain (the strongest predictor of future episodes)
- Age-related changes in the spine
The good news is that most of the modifiable factors respond well to physiotherapy, exercise, and lifestyle adjustments.
What You Can Do at Home for Lower Back Pain
Professional treatment accelerates recovery, but there’s plenty you can do between appointments too:

Stay active. This is consistently the number one recommendation from back pain research. The 2022 Low Back Pain Clinical Care Standard, endorsed by 19 professional associations in Australia, places early activity at the centre of recovery. Gentle walking, swimming, or whatever movement feels comfortable helps keep your back mobile and reduces stiffness.

Break up long periods of sitting. Set a timer if you need to. Stand, stretch, or walk for a couple of minutes every 30 to 45 minutes.

Prioritise sleep. Poor sleep amplifies pain. If back pain is disrupting your sleep, talk to your physio about positioning strategies that might help.

Manage stress. Stress doesn't cause back pain on its own, but it does lower your pain threshold and make symptoms feel worse. Even small changes, like getting outside more or taking breaks during the workday, can help.

Build long-term strength. The people who do best with lower back pain are the ones who commit to progressive strengthening over months, not just weeks. This builds the resilience your back needs to handle daily demands.
When to See a Physio for Lower Back Pain
Book an appointment if you’re experiencing:
- Pain that has lasted more than one to two weeks without improving
- Recurrent flare-ups that keep disrupting your routine
- Pain that limits your ability to work, sleep, exercise, or manage daily tasks
- Sciatic symptoms, including pain, numbness, or tingling into the leg
You don’t need a GP referral to see a physiotherapist in Australia.
When It May Be Serious
Seek immediate medical attention if you experience:
- Loss of bladder or bowel control
- Severe or worsening weakness in one or both legs
- Numbness in the saddle region (inner thighs, groin, buttocks)
- Pain following significant trauma (such as a fall or accident)
- Unexplained weight loss or a personal history of cancer
These presentations are uncommon, but they require prompt investigation.
Get Support for Lower Back Pain
Physiotherapists Mentone
If lower back pain is affecting your comfort or confidence in movement, early support can make a real difference.
mhealth is located in Mentone and services the surrounding suburbs including Beaumaris, Parkdale, Black Rock, Sandringham, Cheltenham, Mordialloc, and Chelsea. Book an appointment with mhealth or contact our team to find out how we can help.
Not Sure If This Is the Right Page?
You don’t need a confirmed diagnosis to book an appointment. If you’re experiencing pain, stiffness, or movement issues and aren’t sure what’s causing them, our team can help assess your symptoms and guide you in the right direction.